“I’m Leaving On a Jet Plane………..”. Bring Narcan
Is there a Doctor onboard? Those dreaded words. Here’s what you get to look forward to?
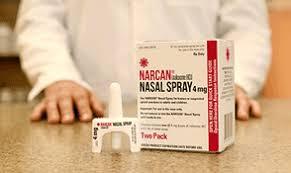
“Delta Air Lines has announced it will begin carrying a drug used to reverse opioid overdoses on every plane after a passenger reportedly died on a flight earlier this month.”
Now an extension of the opiate epidemic, overdoses on board planes are happening, and if ever summoned, physicians will have to include this in the differential. In a sense having Narcan available, this makes sense. In terms of liability, treating an overdose at 10,000 feet presents certain risks. Do the risks outweigh the benefits? Make your own determination. I would welcome the Narcan if the plane kit contained it. However, what if the overdose was severe such that the Narcan was ineffective would there be liability for the physician? “Narcan is a nasal spray that has been proven to reverse opioid overdoses and save lives when the drug is quickly administered to a patient.” But we all know the potency of opiates and amount of opiates being used is significant and increased. Narcan may in fact not be enough to reverse certain severe overdoses. In a sense the notion that the opiate epidemic has progressed to needing Narcan on flights is sad. This is what it has come too. Like it or not, if you are on board and they request for a doctor, physicians are now in the position to have to treat something they might not be comfortable with or have expertise with. I would hate to be in this position, but the reality is that drug addicts will fly and will overdose on planes. To the extent that planes all now carry AED’s, now carrying Narcan is a sign of the times and the next step towards saving lives.









PS: Here’s what I got in the mail:
Hello
Sucker,You are approaching the MOC curriculums learning schedule end date with the following courses not yet completed. Please login to complete these items in the To Do section of the MOC curriculum to stay current. MOC Curriculum: RQI BLS Course Name Due Date RQI Manikin Activity – Adult and Child Compressions and Ventilations Sunday, June 30, 2019
I last did BLS in May 2019, so I’m no longer competent and current in my MOC. WTF MOC? I haven’t the slightest. They know this is a horror buzzword for docs.
But, Bobby, just don’t fail. Out-of-hospital resuscitation comes with a dismal 11% survival, and the American Heart Association is trying to find out whose fault is that.
“Poor-Quality CPR is a Preventable Harm,” states the American Heart Association here.
Any good malpractice attorney can tell you that harm is “to damage, injure or hurt.” According to the British Medical Journal, the rate of deaths in the US due to preventable medical error by hospitals and physicians makes it the #3 cause of death.
The American Heart Association has endorsed the standard that BLS should be practiced every 90 days for a person to remain proficient in BLS/CPR. If it greater than 90 days, the AHA will no longer verify your competence in BLS/CPR, and hold you deficient in your BLS Maintenance of Certification. It sure sounds like stuff I’m making up, but I’m not.
So if you jump up on the plain, remember you have an 88% chance of being held in suspicion for harming the patient with poor-quality CPR; and the American Heart Association will likely hold your CPR competence under suspicion.
When in doubt, don’t touch the patient.
A fascinating study on the overestimation of preventable deaths is shown here.
Steve, that’s a brilliant, factual (“evidence-based!!!”) take. On two occasions I have been sued and settled against for keeping a patient alive after they had coded in the field, and in both cases the family told egregious lies in deposition. I’m sorry if I hurt the sensibilities of more optimistic colleagues, or bum out student hopefuls, but every patient and/or their family is a potential assailant: all they need is a bad outcome, which is very often out of the control of the physician. The sad fact is that limiting exposure to probable bad outcomes – as Steve demonstrates – limits personal risk. I’d probably jump up and help on the plane, because of the guilt I’d feel later if I didn’t; even so, I’d remain angry at myself for voluntarily subjecting myself to risk of legal assault. Between vengeful patients/families and the TSA, I’ll fly as little as possible.