Response to the American Association of Nurse Practitioners

On January 5, 2019 an article entitled, “A Tragic Comedy of Errors” was published in Authentic Medicine in response to a Boston Globe article advocating for the removal of supervisory restrictions on nurse practitioners. Several members of Patient Protection(PPP), frustrated by the lack of objectivity in reporters discussing this topic, decided to write their account of what they have witnessed in their role as patient advocates. Based on their experiences, these physicians believe that nurse practitioners should not be practicing without the supervision of a physician. On January 10, 2019, the article garnered a response by the American Association of Nurse Practitioners (AANP), requesting facts, which are included below:
“The PPP suggests that quality has suffered because of the expansion of NP programs. This is not true. Programs have expanded because of educational and consumer demand. These programs receive certification through such organizations as the Committee on Collegiate Nursing Education. If the PPP has fact-based evidence to show that any of these programs are deficient, it should provide it.”
- Fact: Many NP programs lack structured clinical rotations. Students are responsible for arranging their own clinical rotations. Walden is one example. Walden is accredited by the Committee on Collegiate Nursing Education, the main accrediting agency for nursing programs.
- Fact: There are NP programs that have 100% acceptance rates.
- Fact: There are entry-level NP programs that allow students without nursing degrees to obtain their BSN/FNP degrees. No nursing experience required.
- Fact: The current president of the AANP tacitly acknowledges that there are
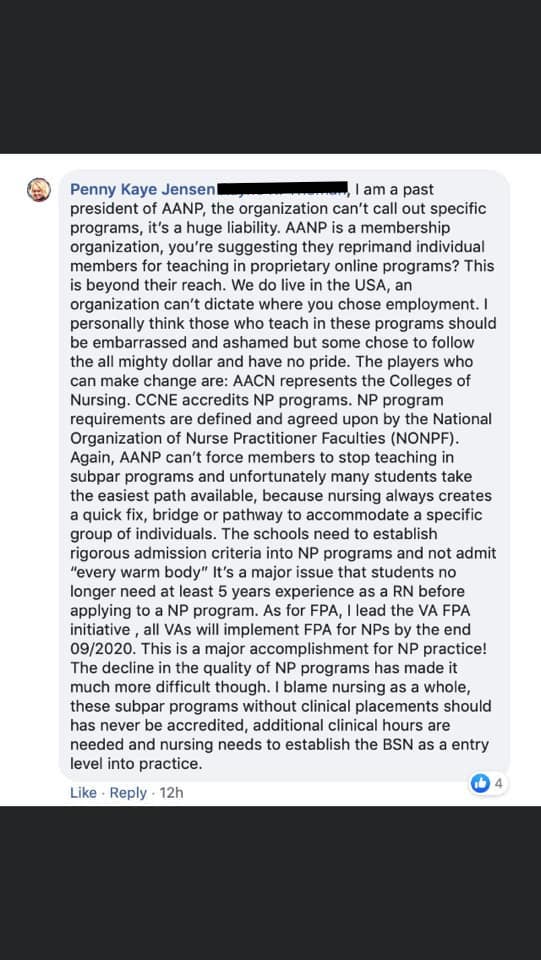
NPs who have knowledge deficits. She suggests they not expose those deficits on social media. - Fact: A former past president of the AANP, Penny Kaye Jensen, DNP, has acknowledged that subpar programs exist.
“In 22 states and the District of Columbia, NPs are granted full practice authority. In the remaining states, NPs are required to contract with a physician under the guise of “supervision” or “collaboration” and, in many cases, must pay a fee to the physician. This is not a health benefit to patients. It is an economic incentive for physicians to boost their incomes while squeezing the supply of providers available to patients.”
- The fact that full practice authority is granted in 22 states and D.C. is more indicative of excellent lobbying than stellar clinical practice since most legislators are unaware of the differences in education between physicians and nurse practitioners. Legislators believe the data presented to them and have chosen to accept poorly done studies as “proof” of equal clinical outcomes.
- The requirements for “collaboration” are generally mandated by the state or the nurse’s malpractice insurance. “Collaboration” is often a way to transfer risk onto the shoulders of a physician. PPP does not agree with physicians who take advantage of supervisory relationships. However,
NPs should not agree to enter into contracts with unethical individuals. They have a choice.
“Most NPs work collegially with physicians. Organizations such as PPP go on the offensive because they fear losing their economic stranglehold over health care.”
- FACT: Several PPP members have private practices in which they employ nurse practitioners (NPs) and physician assistants(PAs). Many members of PPP are retired physicians who no longer have economic employment interests. PPP is not anti-NP, we are pro-patient. As stated clearly in the article, the formation of PPP was a result of mismanaged patients who were subsequently managed by physicians who became PPP members because of their concern for patients.
“The authors suggest several examples of what they believe to be inappropriate care by NPs. Rather than provide specific examples with the final dispositions of these cases in a well-documented fashion, they provide vague information with no specific facts. This is a very slippery slope for medicine, and with 7.4% of physicians experiencing a malpractice claim, compared to just 1.1% of NPs.”
- As explained by the disclaimer in the article, details have been changed to protect the identity of the patient or patients. Each case presented does indicate
final disposition. Asterisks specify how the medical standard was not met. It is important to note that nurse practitioners are not held to the medicals standard as they are nurses and not physicians. The malpractice data presented is extremely vague and does not indicate whether the claims involving physicians were a result of malpractice or negligence bya NP under their supervision. It is no secret that physicians are the preferred targets of malpractice attorneys as the financial return expected is much greater than that of NPs, even if the NP is the primary source or cause of the malpractice/negligence/injury.
“It would be easy to find thousands of documented cases of physician malpractice, including citations from medical boards where physician licenses were suspended or revoked, as well as the disposition of medical malpractice cases where physicians have been sued for millions of dollars.”
- This statement is correct. And every single one of those citations
are public because those physicians HAVE BEEN HELD ACCOUNTABLE. The cases presented in the Authentic Medicine article are cases that might not have been reported had the physician seeing the patient not been a PPP member.
“Some of the physicians who attach their names to this article include Adil Manzoor, DO, and Errin Weisman, DO. These Doctors of Osteopathy should know better. It wasn’t long ago that the American Medical Association (AMA) shunned DOs. In his article published in 2019, Dr. Manzoor appears to stake a claim about the importance of making money as opposed to pushing for quality patient care (“Why I’m Working 30 Hours or Less After Residency”).”
- This is an inappropriate comment and unwarranted attack. Not only did these two physicians not contribute to this article, neither are member of PPP. Doctors of Osteopathic Medicine are physicians and any comparison to nurse practitioners and their experiences with the AMA is unfounded.
- Physicians for Patient Protection is a
physicians advocacy organization who supports physician-led medicine. We believe this to be the best and safest model for patients as physicians are the only health care professionals trained and licensed to practice medicine. In addition, we do not support full practice authority(FPA) or “independent” practice for nurse practitioners. - In our opinion, it is irresponsible for any nursing association, physician organization or legislators to support this edict(FPA) knowing that the nursing educational standards are inconsistent and non-standardized. Currently, there is no process by which nurse practitioners trained at sub-par institutions can be filtered and prevented from practicing independently. Because no clearly delineated guidelines or procedures exist, there is no possible way for patients to protect themselves unless they ask very specific questions.
- The onus should not be on patients to create the process. All health care professionals have a responsibility to the public to protect their patients’ well-being. For this reason, maintaining quality, consistent, educational standards at appropriately accredited institutions is imperative.
**Although the American Association of Nurse Practitioners participated in discussions regarding the recommendation by the American Association of Colleges of Nursing (AACN) to convert the terminal master’s degree to the doctorate of nursing practice(DNP) degree by 2015, they DID NOT mandate it. On 4/20/18, the National Organization of Nurse Practitioner Faculties(NONPF) “made the commitment to move all entry-level nurse practitioner (NP) education to the DNP degree by 2025.”https://cdn.ymaws.com/www.nonpf.org/resource/resmgr/dnp/v3_05.2018_NONPF_DNP_Stateme.pdf. The authors apologize for any misunderstanding resulting from our previous statement in the article, a “Tragic Comedy of Errors”.
**The original response to the Authentic Medicine article by the AANP has been edited. This reply, by select members of PPP, is based on that original response on January 10, 2019.
Get our awesome newsletter by signing up here. We don’t give your email out and we won’t spam you









Perhaps some language in the Practice Act that Nurse Practitioners should practice at a physician standard of care?
As a non clinician who has worked with NP and PA professional associations, I have always been more comfortable with the PA model of working with and under the supervision of physicians.
On the other hand we live in a world where naturopaths, chiropractors and others are licensed to practice. It would be interesting to analyze the independent practice of NPs within that context.
Agree with response! PPP has logic and accruing patient examples on their side. The results of this “experiment” on human lives is beginning to come out. The AANP better raise standards to protect patients.
Payouts for NP malpractice claims increasing (2017)
https://www.fiercehealthcare.com/finance/malpractice-claims-nurse-practitioners- payouts-are-increasing-opioids
“Many malpractice cases in primary care or family medicine were related to a nurse practitioner’s failure to order a medical test, or to obtain and address test results… The report also found that claims related to improper prescribing and management of controlled drugs… increased by about 13%”
Concerns about Variability of Nurse Training and Competency
“The First U.S. Study on Nurses’ Evidence-Based Practice Competencies Indicates Major Deficits That Threaten Healthcare Quality, Safety, and Patient Outcomes.” Worldviews on Evidence-Based Nursing, 2018; 15:1, 16–25
“Tremendous variability in EBP (Evidence Based Practice) persists throughout the United States even though research supports that implementation of EBP leads to high-quality cost-effective care.” Results showed: “There is a tremendous need to enhance nurses’ skills so that they achieve competency in EBP in order to ensure the highest quality of care and best population health outcomes.”
Results *are*
Unbroken link here:
https://www.fiercehealthcare.com/finance/malpractice-claims-nurse-practitioners-payouts-are-increasing-opioids