Crap Shoot: FTC supports bills bolstering advanced practice nurse autonomy

A ‘crap shoot’ is defined as a risky or uncertain matter or something that has an unpredictable outcome. The studies referenced in this article could be called a crap shoot. By this I mean, they don’t provide the evidence they are purported to in support of full practice authority. This article (1) references a 2014 document from the FTC (2) called Policy Perspectives: Competition and the Regulation of Advanced Practice Nurses. The main reasons both the article (1) and the FTC paper (2) drew my attention are:
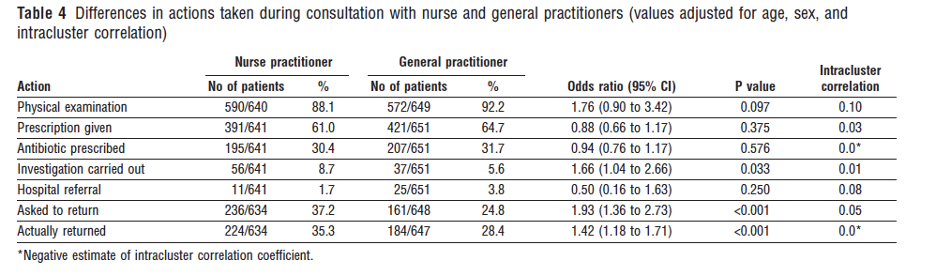
“the FTC pointed to research indicating that advanced practice RNs are as safe and effective as independent doctors and that autonomous advanced practice RNs and doctors have comparable prescribing patterns and ultimately patient outcomes (3).” However, this article is 20 years old first of all. It is based in England and Wales. APRN’s in the study were part of physician led teams. Misinterpretation of date – the study itself reported “Nurse practitioners issued fewer prescriptions than general practitioners, but the difference was not significant”– but this became interpreted as comparable prescribing patterns. The follow up time was 2 weeks – “There were no differences in health status at the end of two weeks.” Next, you judge the stats:
“the FTC cited research from the Institute of Medicine and FTC staff urging state legislators to avoid imposing restrictions on advanced practice RNs’ scope of practice because they are “safe and effective as independent providers of many healthcare services within the scope of their training, licensure, certification and current practice.”(4)” I’ve written about this reference before. The Institute of Medicine (IOM) report (4). Not a credible evidence source. See: https://authenticmedicine.com/2019/05/a-commentary-on-as-nurse-practitioners-try-to-shake-free-of-doctors-kansasphysicians-resist/
“Studies have examined outcomes associated with APRNs with independent prescribing authority, and the results have suggested comparable outcomes between APRNs and physicians (3,5).” This reference is the now infamous Mundinger study (5). I’ve written about this previously debunking this as credible evidence. See:
“studies showed that [APRN]-provided care is comparable to physician-provided care on several process and outcome measures” (6)” This reference is from the National Governors Association: The Role of Nurse Practitioners in Meeting Increasing Demand for Primary Care (6). This reference itself is not a study but more of a synthesis of research. However, some of the studies referenced in it is suspect. For example, the infamous Mundinger study is referenced again here. The Institute of Medicine report is also referenced. The list of references is extensive and would take some time to review, but here’s the list nonetheless (sorry it’s small and hard to read). The full list can be found from the link below:

“research suggests that [APRNs] can perform a subset of primary care services as well as or better than physicians.”(7)” This 10 year old references is an article titled The Role of Nurse Practitioners in Reinventing Primary Care and is a summary of available evidence of nurse practitioner contributions to improving primary care and reducing more costly health resource use. Guess which reference is in this article?? Yep – Mundinger. This article also states the infamous “substantial barriers prevent nurse practitioners from practicing to their fullest capabilities.” What does this even mean? This is never defined in this article nor in the literature. It’s arbitrary rhetoric for full practice authority. In other words, a strawman (https://authenticmedicine.com/straw-man-the-dishonesty-needs-to-stop/). See the references section for a full list of studies they reviewed. The limitations in the article are telling:
Bias – “the search terminology and exclusion criteria may have unintentionally influenced the body of evidence we examined.”
Questionable quality studies – “the quality of the studies retained in this review is uneven.”
“four studies included in this review were conducted outside the United States”
“regarding the economic impact of NPs are limited by the small number of U.S. studies comparing costs, methodological concerns, and questions regarding the assumptions on which these analyses are based.”
References:
- https://www.modernhealthcare.com/providers/ftc-supports-bills-bolstering-advanced-practice-nurse-autonomy?utm_source=promote-editorial&utm_medium=email&utm_campaign=Evergreen-Care-Delivery&utm_term=Article1&utm_content=06072020
- https://www.ftc.gov/system/files/documents/reports/policy-perspectives-competition-regulation-advanced-practice-nurses/140307aprnpolicypaper.pdf?utm_source=govdelivery
- P. Venning et al., Randomised Controlled Trial Comparing Cost Effectiveness of General Practitioners and Nurse Practitioners in Primary Care, 320 BMJ 1048 (2000) (no significant difference in patterns of prescribing or health status outcome);
- Inst. of Med., Nat’l Acad. of Sciences, The Future of Nursing: Leading Change, Advancing Health 98-103, 157- 61 annex 3-1 (2011)
- Mundinger et al., Primary Care Outcomes in Patients Treated by Nurse Practitioners or Physicians: A randomized Trial, 283 JAMA 59 (2000);
- Nat’l Governors Ass’n, NGAPaper: The Role of Nurse Practitioners in Meeting Increasing Demand for Primary Care (2012), http://www.nga.org/files/live/sites/NGA/files/pdf/1212NursePractitionersPaper.pdf
- Mary Naylor and Ellen T. Kurtzman, The Role of Nurse Practitioners in Reinventing Primary Care, 29 Health Affairs 893, 894-5 (2010). https://www.healthaffairs.org/doi/pdf/10.1377/hlthaff.2010.0440









Let’s just be politically correct and call everybody who wears scrubs or a white jacket a health care provider…….we all generate RVU’s by providing CPT’s.
The legislators say we do the same work, the hospital administrators say we do the same work, heck some of our brethren say we do the same work.
We all just want happy patients and we all want RVU’s (and 5 star social media ratings)
There are still a few savvy patients out there who do check my CV….bravo for them!
The next generation needs to accommodate to Third World medicine, corporate-to-consumer treatment. Put the bigggest idiots in charge and let them strut. I favor changing the terms te EMT-MD. SO WHAT? Counterfeit is counterfeit.
The next generation needs to accommodate to Third World medicine, corporate-to-consumer treatment. Put the bigggest idiots in charge and let them strut. I favor changing the terms te EMT-MD. SO WHAT? Counterfeit is counterfeit.
Nurse Practitioners are not educated to be responsible for emergency care of patients. They will and are missing diagnosis and treatments tht are costing lives. They do have a place in the medical community and would serve a great need in the rural hospitals and clinics, but not in the care of critical every second counts patients.