The Velvet Rope of Narrow Networks
The insurers love the concept of narrowing networks. Here, from the WSJ, is what the plan is:
Offering a smaller selection of health-care providers holds down costs, in part because hospitals and specialists with the highest reimbursement rates can be cut out. Insurers now increasingly strike special deals with providers that aim to incentivize more efficient and high-quality care. HMOs often also include hurdles to care, such as requiring a referral in order to see a specialist.
This is about money. This is about control.
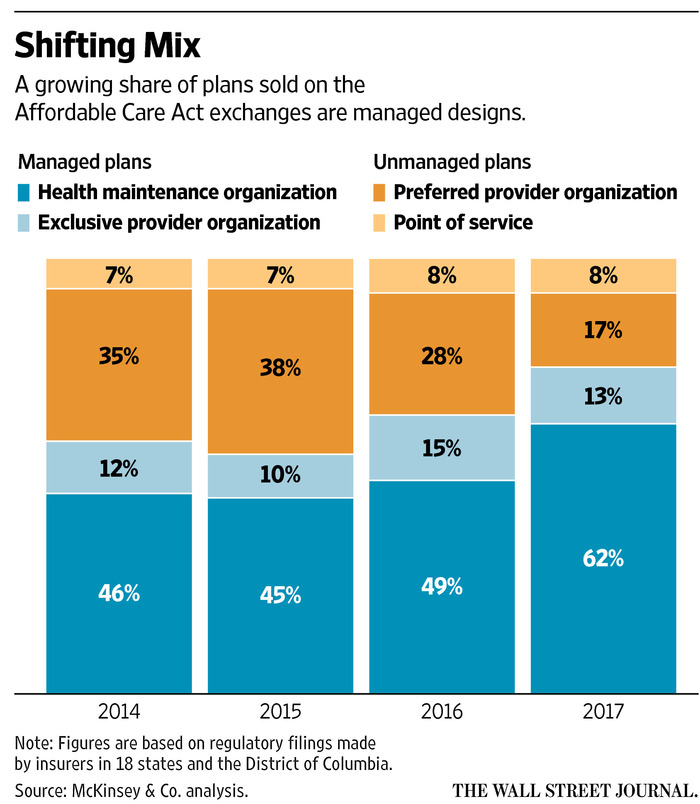
A new term being used is EPO or “exclusive provider organization”. Brilliant euphemism. It has that velvet rope connotation but is just the opposite. When you see EPO think “narrow network”, which means you lose total control of who you can see. This is the trend we expect to see:
In Washington, Premera Blue Cross said it will next year stop selling PPO plans that had enrolled 49,100 on the state’s exchange. Instead, Premera will offer EPOs that don’t include out-of-network coverage.
People criticize Obamacare for gouging the middle class in taxes, for helping the insurers raise rates and for making deductibles unreachable but they forget the cherry on top, which are these narrow networks. Nice work.









Kiss goodbye to quality and personal commitment … Oh wait – too far gone already; maybe a feeble wave. One must remember that when it’s about Money and Control, it’s ALL about Money and Control. Replace value and patient or community health outcome with surrogate and easily manipulated metrics, key payment to clicks and not honest work, talk Team when you really want a subservient Flashmob, remove the patient and community from freedom of choice and meaningful economic input and you will get bloated, indifferent and wealthy management empires, an alienated workforce whose successors will be obedient serfs who punch a clock and click a box by rote. And the Public – pay more and get less.
-These changes are taking place in the face of an economy that is damaged in general. The real unemployment rate (as per shadowstats) is well into the two digits, not the phony 5% touted by the Government. The real inflation rate’s about 5-6%, not the bogus baseline of 1%-2% that the Government offers. The economy has been kept afloat by several incidentals, not the least of which is the boom of oil, and the collapse of oil prices, by fractional extraction.
-Look back at the August 31 authenticmedicine post, friends. The only way that the middle class is staying afloat, is by the DEFLATIONARY trend of goods such as clothing, that have dropped in price over the last half-dozen years. Look at the graph.
-Stuff that can be deflated by shipping its production offshore to Indonesia, like clothing, has help push down the real price of things. Wal-Mart business methods have also cut down on the real price of things. Because Wal-Mart owns a huge captive market, they dictate the prices they will pay the producers – and they’re not generous. If someone can make lawn furniture for five cents cheaper, you’re fired from the supply business, pal.
-Some businesses can be crushed into efficiency by the Wal-Mart technique; and some can’t. -Strangling the networks for HMO’s is the same gig Wal-Mart offers its producers. Take it or leave it. I give it about three years when we start extensively “offshoring” surgeries to Mexico and the Caribbean. Let’m compete on a global market! Besides, the American physician’s going the way of the Zenith Tube Radio. The other cost component on the graph is the exploding bureaucracy of medicine – that’s got to account for some of the 3-5% annual rise in healthcare.
-Think of it. If REAL inflation’s siphoning off 5% per year, and healthcare costs are rolling up slower than that, at 3.5%, AND the bureaucracy’s expanding, who’s making up for the balance sheet? I’m seeing about a 5% or more DEFLATION of expendables like salaries.
-There was a reason Grandpa dreaded deflation. In the Great Depression, wages and prices dropped. But as the wages go down, demand goes down, and the amount of dollars available to circulate in the economy goes down. That’s why the plan used to be to avoid economic deflation. Since about 2000, the Government’s been speedily burying the deflation under a rug, and blaming it ALL of the healthcare sector. Stop medical greed! Billions spent! Yes, of course. -But the money’s not under the doctors’ mattresses. Until we “offshore” medicine, we’re in a pickle.
-Military potentates from horrible festering African totalitarian states used to send their relatives to the United States for medical care. That didn’t speak well of the culture and economy of their horrid little fiefdom. And in five years, we’ll be sending people to Mexico and the Caribbean for medical care. What’s that say about us?
We are constantly approached to join these organizations. We had been immune for quite some time due to our rural status, which gave us some independence and power. Now, as those around us fold, my partners are getting nervous. My question is always the same. “How does this help our patients?” No answer, but some mumbled garbage about quality care. And that we are already doing these things, why not get paid for it. It makes me laugh/cry/curse. They are trolls, digging into the center of the mountain, looking for their gold (data). And now, they want us to go into the dark with them. These insurers don’t provide health care. We do. Sorry, this was a rambling mess. This post came at the perfect time. Thanks
Hardly a rambling mess, for sure. You’re just saying what the rational marketplace does when those that DO to those that DEMAND. How can one measure and prioritize demand, without the market price? Bureaucrats claim the power but not the ability. The next move is physical threats and legal intimidation. But that can’t help either. The end game is arriving.