The Joys of Health Insurance Bureaucracy by Val Jones MD
From a health perspective, I am grateful to be doing well. I only have one active medical condition that is fully treated by one prescription medicine. I have been taking this medicine since I was 18 years old. I recently bought myself a personal health insurance plan (my first that was not tied to employment) and simply wanted to resume regular purchase and use of my medicine.
I was pleased to note that purchasing my medicine through my new insurance plan would save me a little bit of money (about $25/month). So I presented my card at my local pharmacy and was told that my medicine was not covered under my plan without pre-authorization from my doctor. I called my pharmacy benefits hotline and had them send a pre-auth form to my doctor. Then I asked my doctor to fill out the form and fax it back. That was over three months ago.
When I called to inquire about the pre-auth forms, the benefits folks told me that they had no record of the fax. So I asked my doctor to send another fax form and I waited another week. When I called the benefits people, they again said that they had no record of the pre-auth documentation. They also said that I could not be transferred to the pre-auth team to figure out why it was missing (wrong fax number perhaps?) because they only speak to physicians.
So out of curiosity I asked what the usual process was for obtaining a prescription medication once it has been authorized. The benefits staff didn’t know. I asked who would know and they said that only the “experts” in the pre-auth department know how medications are obtained by the member after being approved. I wondered how I’d ever figure this out if I wasn’t allowed to speak to them and I was told that I might be able to get an answer if I asked a customer care representative to request information on my behalf from the pre-auth experts. But… the pre-auth team was not in the office at the moment and I’d need to call back on Monday. (Parenthetically, the team is physically located in Pittsburgh, though I’m a member in Charleston, South Carolina.)
I asked the benefits team if they generally mail members their meds (I had heard this was the case) or if I could pick them up at my local pharmacy (my preference). They said they didn’t know, but I could call customer care on Monday.
So far, my experience with my new plan – to save $25 dollars/month on one prescription – has cost me 3 months and 1 week of waiting time, two form completion episodes from my doctor, discussions with several pharmacy benefits reps in a state far away from where I live, denial of communication with the only people who know what’s potentially holding up my prescription approval, and about a half hour of completely unhelpful discussion of basic prescription drug purchasing processes that staff at the drug benefits company themselves don’t understand.
And I’m healthy, I’m a healthcare provider who knows how to navigate the system, and I only need one prescription. What do sick people do? (I know, it’s awful out there.)
Life was much simpler when I paid for my medication out-of-pocket without an insurance middle man. I have often wondered if health insurance bureaucracy is purposefully designed to wear patients down to the point where they’ll just pay for things themselves rather than experience the pain associated with getting an insurance company to cover their portion of the cost. (The only other explanation is that health insurance company ineptitude comes from being administrative behemoths with too many moving parts and processes). It’s probably a mix of the two. Or maybe the latter supports the former so there’s no real incentive to pursue true efficiency.
But one thing I did notice – the insurance company was incredibly efficient at figuring out how to direct debit my premiums within 24 hours of signing up for the plan, and have increased my premium once already – by about $25 a month.
You can’t win, my friends.
If you’re healthy, get yourself a high deductible plan, pay as little in premiums as possible, and sock away some money in case of a catastrophic event. Pay cash for your primary care, and do whatever you can to stay healthy and out of the hospital. That’s my plan and I’m sticking to it.
***
Update: My medicine was finally approved/authorized, but I was informed that my doctor would need to send a new Rx form to them before I could receive my prescription. The Rx needed to be on their company’s form, so they had to fax him the request first. I asked how I would pay for the prescription and where I could pick it up and was informed that I’d save about 15% if I agreed to have the medicine mailed to my home (but delivery would take 2 extra weeks).
So I agreed to have it mailed to my home and offered to give them my credit card. They said I should call back with it once my doctor’s Rx had been received. I asked them how I would know when that had occurred. They said that they couldn’t call me to tell me when the Rx had arrived because I had selected “text messaging” as my preferred method of contact, and they don’t inform members of Rx form receipt via text messaging. So I agreed to switch my preference to calls (instead of text), and now I’ll probably get automated prescription refill information in the form of incoming calls on my personal work phone from now till I die. That’s if they don’t sell my phone number to telemarketers in the mean time.
And how annoying is it for my doctor to have sent out two faxes and one new Rx form for ONE prescription (not to mention reading the email explanations from me regarding correct pharmacy benefits plan form usage)? He was uncompensated for his time in this matter…
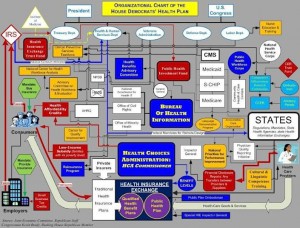









Don’t doubt it’s intentional, and even though I tend Democratic, don’t blame Republicans. As far as I can tell the problem will worsen under Obamacare. Just imagine you’re an insurance company required to charge a low fee to customers you know you’re likely to lose money on, and you know we’ll which customers you’d like to keep. You’re going to offer messages and mammograms to women under 50, keeping their whole healthy family, and good phone service. The calls from the expensive will be routed to a different office where everything goes in circles, or whatever is pricey will be covered if your doctor likes you enough to donate a half hour of their time to the same circles. Friendly doctors who care for the sick will go broke or burn out, and expensive patients will “fire” you, just what you wanted. I’d live to take credit for this insight but it came from a teacher in residency in 1988 who said “HMO’s make money by pissing off the sick”. This has to happen, whatever company pisses off the most sick people will be the winner.
As you and so many others are now starting to see, these private companies are doing this deliberately, and they are laughing all the way to the bank at all the Republican doctors who voted for our Republican “public servants” who are in the pockets of big business, and who let them do whatever the frigin heck they want. I know this for sure because someone I know who used to work for the insurance industry told me so.
Hey folks, lets vote with more wisdom this time around and elect progressives to congress.
Heh, you’re lucky it was that easy. I wish I had the time to tell you the many fun times I’ve had with my insurance company this year. The most fun was when it took 15 months and repeated coordinated joint efforts from me and my pcp’s office to get her paid for one appt (and they’d paid her every time since then, and they had my certificates of creditable insurance on file after I sent them again and again and again and the pcp’s office sent them again and again, but then their claims dept was repeatedly inept with kicking the claims back because nothing was on file or it was a duplicate claim or it was not filed in a timely manner when it had originally been… you get the idea).
Almost as fun was getting a location for an Aurora MRI for a breast cancer recurrence scare while this was going on, with the insurance company not wanting to talk with me since I’m not a physician AND not wanting to talk with the physician’s office for some reason (the office manager is only the physician’s wife so wouldn’t know what’s going on at all). The insurance company gave me their list of six recommended locations (none of which had the special machine needed), and then finding location #10 for me to go to days later, which was the one my surgeon’s office tried to get them to get me to 10 days prior when this all started, which would’ve been no problem had the insurance company been communicating with the office in the first place…. :-/
I’m still waiting for them to pay my chiropractor for all visits from last November to present. Not holding my breath there.
At least this company is better than one I had several years ago, which thanks to a typo, got 1/4 of my yearly salary that year thanks to my having to pay retail after the $500/year covered by the plan (not $5,000) on top of paying about $72 each week via payroll deduction for the privilege of paying retail, on top of paying for all meds after the first $50 each month. :-/
Yesterday UnitedHealth announced 3rd quarter profits of $1.56 BILLION. It’s coming from the pockets of providers and consumers like this example.
Physicians should lobby Congress for the ability to submit charges to these pharmacies for the time it takes to fill out their numerous copies of the same thing and fax it three times.
I suspect these charges would just about cover the Medicare “adjustment” to practitioners claims.
Nice column, good points.